Endoscopic spine surgery is an alternative to conventional open microdiscectomy surgery that can be considered for certain types of herniated disc. Endoscopic surgery is a minimally invasive surgical treatment, and as such, has the advantages of reducing the manipulation of soft tissues, bone and ligament structures, which means less postoperative pain, and no destabilizing effect on the lumbar spine.
WHAT CASES IS IT USED FOR?
Endoscopic surgery of the lumbar spine is indicated for certain pathologies:
- Foraminal disc herniation
- Extraforaminal disc herniation
- Posterolateral or medial disc herniation
- Foraminal stenosis
- Central canal stenosis
On the other hand, this type of intervention is not recommended in case of bulky or migrated hernias, calcified, or with spondylolisthesis.
WHAT DOES THE PROCEDURE INVOLVE?
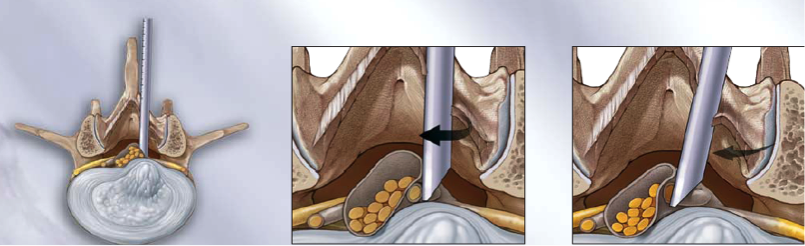
Lumbar endoscopic discectomy is performed through a 5-8 mm incision in the skin. Through the incision, a cannula is inserted until reaching the vertebral disc through the neural foramen (in the case of foraminal or extraforaminal hernias) or the interlaminar space (posterolateral or medial hernias), depending on the location of the hernia to be treated.
Through this same cannula, first the optical camera that allows the surgeon to view the enlarged field of work on a screen is introduced, and then, the instruments that will be used to extract the herniated disc tissue and decompress the nerve. The delicate internal tissues are constantly irrigated through the cannula throughout the surgery, which makes it possible to control or stop bleeding and dissection of the structures.
Several studies have shown that endoscopic spine surgery has the following advantages when compared to conventional surgery:
- Less postoperative pain thanks to the lesser manipulation of tissues.
- Less blood loss.
- Lower risk of cerebrospinal fluid (CSF) fistula.
- Causes no instability, as in many cases it is not necessary to remove any bone to reach the hernia.
- Procedure is performed under local anesthesia and sedation, eliminating risks associated with general anesthesia.
- Enables a swift return to work.
RECOVERY AND REHABILITATION AFTER AN ENDOSCOPIC LUMBAR SURGERY
As it is a minimally invasive surgery, the recovery is faster when compared to traditional surgeries. The patients can get up and walk the same day of the operation, and in a large percentage of cases, they need only 1 night in the hospital.
The average recovery time is 3-6 weeks. Rehabilitation and physiotherapy are not required because there has been little manipulation of the tissues and bones during the procedure, so postoperative pain is significantly reduced.
RISKS
The possible risks and complications of endoscopic surgery are similar to those of conventional surgery. We review them below:
Immediate
Damage to neurovascular elements or to the abdominal-pelvic structures, insufficient decompression.
Short term
Dysesthesia, hematoma, infection, CSF fistula.
Long term
Reherniation or instability at the operated level.